03/04/2026
Vitrectomy Surgery
For many patients, the first indication that something is wrong inside the eye is not pain, but a change in the quality of vision. Straight lines may appear distorted, floaters may increase suddenly, or vision may blur in a way that does not improve with blinking or glasses. In some cases, the presentation is more acute, such as a sudden drop in vision from vitreous hemorrhage or symptoms suggestive of retinal traction or detachment.
These are the clinical scenarios in which vitrectomy becomes relevant. As a cornerstone of modern retina surgery, vitrectomy has transformed the management of a wide range of vitreoretinal disorders. Today, vitrectomy surgery and the broader field of eye vitreous surgery are integral to advanced ophthalmic care, offering patients access to highly specialized treatment for complex retinal disease. Centers such as Barraquer Eye Hospital have developed dedicated vitreoretinal services designed to provide timely diagnosis and intervention in these cases.
What is vitrectomy?
Vitrectomy, or pars plana vitrectomy, is an intraocular microsurgical procedure in which the vitreous gel is removed from the eye. The vitreous is a transparent, gel-like structure that fills the posterior segment and contributes to the eye’s internal architecture. With age or disease, however, it may become pathological contracting, opacifying, hemorrhaging, or exerting traction on the retina.
Once the vitreous becomes part of the disease process, surgical removal allows direct access to the retina and vitreoretinal interface. Vitrectomy therefore serves both a therapeutic and a facilitating role: it eliminates pathological vitreous and enables precise treatment of underlying retinal pathology.
This dual function explains why vitrectomy is central not only to eye vitreous surgery, but also to contemporary retina surgery as a whole.
When is vitrectomy indicated?
Vitrectomy is indicated in a broad spectrum of retinal and vitreous conditions. Common indications include retinal detachment, vitreous hemorrhage, epiretinal membrane, macular hole, complications of diabetic retinopathy, retained intraocular lens fragments, and ocular trauma.
In retinal detachment, vitrectomy is used to relieve vitreoretinal traction, identify and treat retinal breaks, and facilitate reattachment. In diabetic retinopathy, it may be required to clear persistent vitreous hemorrhage or to remove fibrovascular membranes causing tractional changes. In macular disorders such as epiretinal membrane and macular hole, the procedure enables delicate peeling of pathological tissue to restore retinal architecture.
In many of these situations, the objective is to repair retina anatomy before irreversible functional damage occurs. In others, the aim is to clear the visual axis or stabilize progressive disease. The indication is therefore individualized, and careful patient selection is essential.
At Barraquer Eye Hospital, surgical planning is tailored to the underlying pathology, with emphasis on both anatomical success and functional outcome.
Why vitrectomy has become central to retina surgery
The role of vitrectomy has expanded significantly over recent years, driven by advances in surgical instrumentation, visualization systems, and intraoperative control. Modern small-gauge vitrectomy systems typically 23-, 25 -, or 27-gauge allow surgeons to operate through self-sealing microincisions with minimal disruption to ocular tissues.
For patients, this generally translates into reduced postoperative inflammation, improved safety, and faster recovery. For surgeons, it enables greater precision when addressing complex vitreoretinal pathology.
As a result, vitrectomy surgery in our city Dubai is now routinely performed in specialized centers, including Barraquer Eye Hospital, where access to advanced technology and experienced vitreoretinal surgeons supports high-quality care.
How the procedure is performed
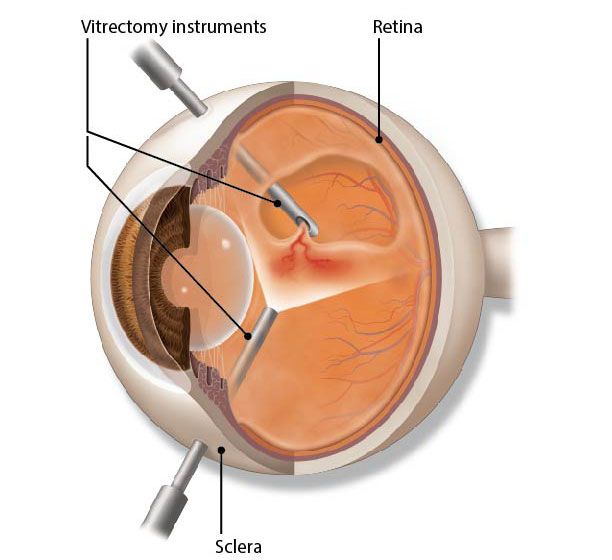
Although technically complex, vitrectomy follows a structured sequence. After appropriate anesthesia most commonly local anesthesia with sedation the surgeon creates small entry ports in the pars plana region of the sclera. Through these, microsurgical instruments are introduced into the vitreous cavity.
The vitreous gel is then removed using a high-speed vitreous cutter. This step may itself restore vision in cases of dense vitreous opacities or hemorrhage. More commonly, it allows access to treat the underlying retinal condition.
If retinal detachment is present, the retina is reattached and retinal breaks are sealed using endolaser photocoagulation or cryotherapy. In macular surgery, membranes such as epiretinal tissue or internal limiting membrane may be peeled under high magnification. In diabetic eye disease, tractional membranes are carefully dissected and removed.
At the conclusion of the procedure, the vitreous cavity is filled with a tamponade agent when required, to support retinal healing.
Gas and silicone oil: the role of internal tamponade
Internal tamponade is a critical component of many vitrectomy procedures. Gas bubbles are frequently used in retinal detachment and macular hole surgery, acting as a temporary internal support that holds the retina in place while healing occurs. The type of gas used depends on the desired duration of tamponade.
Silicone oil may be selected in more complex cases requiring longer-term support, such as advanced proliferative vitreoretinopathy or certain traumatic detachments. Unlike gas, silicone oil does not resorb spontaneously and typically requires a secondary procedure for removal.
Patients undergoing eye vitreous surgery with gas tamponade must follow specific postoperative precautions, including avoiding air travel and maintaining prescribed head positioning when indicated. These measures are essential to optimize the outcome of retina repair.
Recovery after vitrectomy
Recovery after vitrectomy varies depending on the indication and the complexity of surgery. In the immediate postoperative period, patients commonly experience blurred vision, conjunctival redness, mild discomfort, and light sensitivity. If a gas bubble is present, vision will remain limited until it gradually resorbs.
Over the following weeks, inflammation subsides and visual function begins to improve. Patients are typically treated with topical medications and monitored closely through follow-up visits. Full visual recovery, when achievable, may take several months.
It is important to recognize that vitrectomy is often performed not only to improve vision but also to prevent further deterioration. In many cases, stabilizing the condition represents a successful outcome.
Outcomes and expectations
Vitrectomy is a well-established procedure with high anatomical success rates in many indications. However, functional outcomes depend on several factors, including the underlying disease, duration of pathology, and involvement of the macula.
For example, patients undergoing vitrectomy for retinal detachment may achieve excellent outcomes if treated early, particularly when the macula remains attached. In contrast, chronic or complex cases may result in more limited visual recovery despite successful anatomical repair.
Clear preoperative counselling is therefore essential. At Barraquer Eye Hospital, patients are guided through realistic expectations, with emphasis on both the benefits and limitations of surgery.
Why patients seek vitrectomy surgery in Dubai
The demand for vitrectomy surgery in Dubai reflects the region’s growing role as a center for advanced ophthalmic care. Patients benefit from access to specialized retina services, modern surgical platforms, and efficient care pathways.
Within this landscape, institutions such as Barraquer Eye Hospital provide comprehensive vitreoretinal care, combining rapid diagnosis with individualized surgical management. This is particularly important in conditions where timing directly influences prognosis.
The broader field of eye vitreous surgery continues to expand, offering patients access to increasingly sophisticated treatment options across a wide spectrum of retinal disease.
Final thoughts
Vitrectomy remains one of the most important and versatile procedures in modern ophthalmology. Whether the objective is to clear vitreous opacity, relieve traction, or repair retina structure, it provides a highly effective means of addressing complex intraocular pathology.
For patients, early recognition of symptoms and timely access to care are critical. In experienced centers such as Barraquer Eye Hospital, where advanced retina surgery is performed routinely, vitrectomy offers a reliable pathway toward stabilizing or improving vision.
As surgical techniques continue to evolve, outcomes are expected to improve further reinforcing vitrectomy’s central role in the management of vitreoretinal disease in Dubai and across the UAE.
Schedule a consultation today
-
Email: appointments@barraquer.ae
-
Phone (outside UAE): +971 4 573 9999
-
Toll-Free (inside UAE): 800 234 823 (BEHUAE)
-
Working Hours & Location : Click on Google Map Link