09/06/2024
What is Eye allergy?
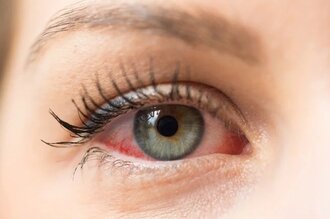
Eye Allergy is a disease that occurs when the eyes react to an irritating trigger (called an allergen). The allergen escalates an immune response and the eyes become red, swollen and itchy. Some allergic conjunctivitis affects both eyes, but asymmetry (one eye more affected than the fellow eye) is not uncommon. Allergic conjunctivitis is not spreading person to person (noncontagious conjunctivitis).
Symptoms:
The symptoms of allergy include red eye, itching, swollen or droopy eyelids , excess mucous in the eye, feeling of foreign body in the eye, and even blurred vision and fluctuating visual acuity.
These symptoms are usually worsening during spring season, exposure to a triggering allergen and dry environment. They are also aggravated when the patient is rubbing the eyelids and has poor hygiene conditions.
Causes and risk factors:
Allergy is caused by a Gene-environment interaction, it means that it is necessary a genetic predisposition but there is an external trigger responsible for the inflammatory response.
The risk factors are host related as heredity, race, gender and age, and environmental factors such as pollution and smoking.
- Family history of allergies increased the risk of ocular allergies. This factor is called Genetic Predisposition, but it is not related to a hereditary pattern.
- Age and gender. Affects equal both sexes, however some types of allergies have male predominance as Vernal keratoconjunctivitis (KC). Ocular allergy could happen at any age group, Vernal KC is common during childhood instead of Atopic KC that affects adults.
- People with eczema, asthma and other allergies are more likely to get any form of ocular allergy.
- Use of contact lenses, and a history of eye surgery when stitches were applied.
- Indoor exposure to active smoking, particularly maternal smoking are important risks factor for Atopy.
- Living or working in an environment that exposes you to allergens.
- A dry environment may worsen Vernal KC while high humidity is related with mold allergy.
Types:
There are 4 types of ocular allergies:
- Seasonal acute allergic conjunctivitis is the typical acute allergy of every spring or related with specific pollen, dust or mold. It is nonvision-threatening and self-limited.
- Giant papillary conjunctivitis is a specific allergy caused by contact lenses or chemicals used to clean them; exposed stitches rubbing against the eyelid and chronic allergies.
- Vernal keratoconjunctivitis is an atopic seasonal recurrent ocular disease caused by allergens such as dust, pollen, animal and food allergens. Usually started during childhood and 23% of the patients may have a chronic perennial form. A personal or family history of atopy is frequently associated.
- Atopic keratoconjunctivitis is a severe and chronic atopy that frequently affects the cornea. The age of onset is the 2nd to 5th decade, and it is associated with atopic dermatitis.
Prevention:
Avoiding the trigger factor is a must. Sometimes the trigger allergen is unknown and limiting the exposure to them with proactive control of the environment is the first step of the treatment. It is recommended to keep your windows closed, vacuum the rugs curtains and soft furniture, wash hard surfaces often and eliminate leaks in pipes, roof and walls.
Some patients must maintain the topical or systemic treatment for years. Adherence to the treatment is a keystone for the long-term control.
Wearing wraparound sunglasses to protect your eyes could alleviate and prevent acute episodes.
Treatment:
Chronic allergy can cause serious damage to your cornea. The cornea is the transparent window of your eye; when it becomes cloudy or irregular, you cannot see clearly. Treatment has 3 objectives: reduce or remove the trigger allergen, alleviate the symptoms of a patient and reduce the eye inflammation.
The treatment involves:
- Avoiding the trigger factor as dust, animal allergens, food allergens and contact lenses in GPC
- Conservative management with cold compresses and lid scrubs.
- Use of anti-allergic eyedrop or ointment prescribed by your ophthalmologist to reduce itching, swelling and inflammation.
- Increasing the lubrication on the eye's surface with artificial tears, mainly preservative-free ones, and in severe cases, the use of blood derivatives from the patient themselves in the form of eyedrops is an option.
- Reduces inflammation of the eye's surface caused by the allergy by using anti-inflammatory eyedrops. The use of this type of drug has side effects like increased intraocular pressure.
- Systemic treatment for severe types or very acute allergies. This systemic treatment should be strictly monitored by a multi-disciplinary team, your ophthalmologist, a GP, an allergist and sometimes an immunologist.
- Immunotherapy for patients with systemic atopic disease as atopic dermatitis and asthma is an option.
Written by:
Dr. Hernan M. Osorio ,
Consultant Ophthalmologist