How cataracts affect colours
20/05/2026
22/11/2023
It provides detailed information about the cornea's curvature, thickness, and shape, playing a crucial role in diagnosing and treating various eye conditions. Irregularities or deformities in the cornea's shape, curvature, or clarity can significantly impact a patient's vision and refraction.
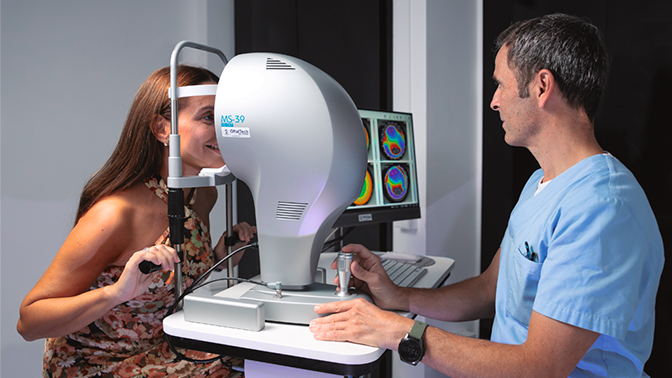
The test utilizes a corneal topographer, available in various types such as reflection, Scheimpflug camera, OCT, and ray tracing. During the examination, the patient rests their chin on a support and focuses on a visible point of light for a few seconds. This process generates precise data on the corneal surface, including elevation, curvature, and corneal thickness maps. The obtained information allows the creation of different maps, whether in three-dimensional or single-plane formats.
To undergo this examination, it is advisable to refrain from using contact lenses for a minimum of 48 hours for soft lenses and 15 days for hard lenses.
Corneal topography plays a crucial role in various clinical scenarios. In the realm of refractive surgery, it proves invaluable for assessing the feasibility of procedures like LASIK, PRK, Smile, or the implantation of phakic intraocular lenses. This assessment takes into account factors such as corneal thickness, shape, and anterior chamber depth.
Additionally, corneal topography serves as a vital tool in both early and advanced detection of corneal pathologies, including conditions like keratoconus or corneal dystrophy. This early identification enables tailored interventions, ranging from intracorneal segment implantation to the application of ultraviolet light, depending on the severity of the case.
In contemporary practice, corneal topographies have assumed heightened significance in the management of astigmatism. This is particularly evident in cataract surgery and refractive procedures involving the transparent crystalline lens, where the information provided guides decisions on the toricity of intraocular lenses.
Francisco Javier Martínez Fuentes, Technician in the Department of Refractive Surgery