How to care for eyelids and treat blepharitis? Effective hygiene tips
29/04/2026
06/10/2015
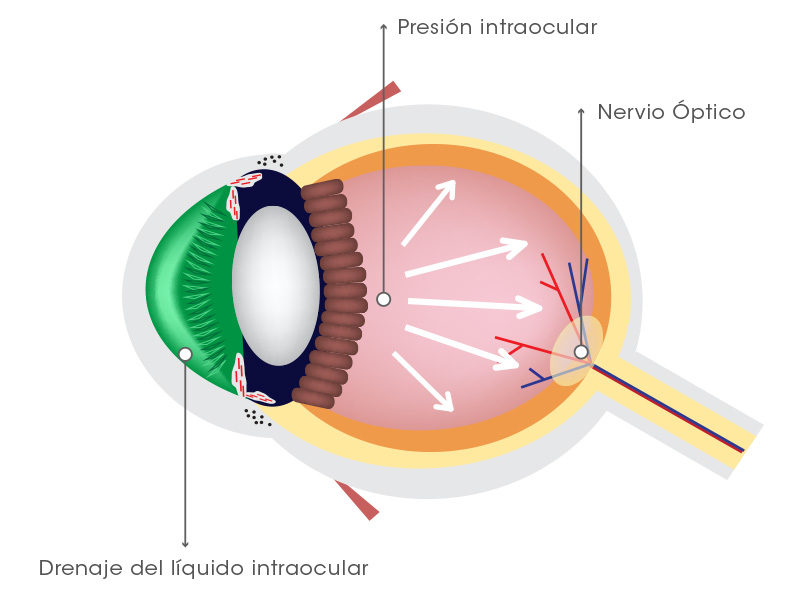
The intraocular pressure (IOP), commonly called "intraocular pressure" refers to the range of measurable pressure inside of the eye.
IOP follows a circadian rhythm that depends on the sleep-wake rhythm. Its maximum lies approximately between 8:00 and 11:00 am, and the minimum between 12:00 and 2:00 am. The oscillation during the day can be up to 3-5 mmHg. In healthy adults the normal IOP range is between 10 and 21 mmHg and has a tendency to increase with age.
There are many techniques to measure the pressure inside the eye, carried by tonometry. Tonometry is based on the relationship between the IOP and the force required to deform the natural shape of the cornea. The measure using the Goldman tonometer represents the most reliable and frequently used by ophthalmologists. This requires topically anesthetize of the cornea, and fluorescein applied on it.
We have other techniques such as;
We should not forget that there are factors that can affect the measurement of IOP as the state of the cornea, the corneal thickness, radius of curvature or degree of hydration, may influenced the measurement.
Also, wear clothing with a narrow neck, overly tight ties, shortness of breath, tightening the eyelids or Valsalva maneuvers may erroneously increase pressure ranges.
A continuous high IOP can damage the optic nerve and may cause glaucoma. Therefore, it is important to perform annual checkups in patients with risk factors of developing it.
In patients with suspected high IOP, measurements can be performed during an entire day, what is known as "curve" of intraocular pressure.